Nervous System Regulation in Session: A Practical Guide to Polyvagal-Informed and Somatic Tools for Therapists
- Apr 21
- 9 min read
The client is describing something that happened three weeks ago. Her voice is steady. She's choosing her words carefully. And when she pauses to collect her thoughts, you notice her jaw has been clenched for the past ten minutes.
She is articulate, self-aware, and genuinely trying. Her nervous system is somewhere else entirely.
This is one of the most common and most important moments in clinical practice: a client who can narrate her experience clearly, but whose body hasn't processed any of it. No cognitive reframe is going to land right now. Not because the insight isn't good. Because the state won't receive it.
Nervous system regulation is the work that creates the conditions for everything else in therapy. This post walks through a polyvagal-informed, somatic approach to that work, built directly from the content inside the Nervous System Toolkit, a 110-page practical workbook that takes therapists and clients through the full arc from ANS basics to trauma responses, somatic practices, and daily regulation rhythms.
A note before we go further: this post uses polyvagal theory as a clinical framework. The scientific picture is genuinely complicated. Some of the biological claims, particularly around the anatomy of the dorsal vagal pathway, have been meaningfully challenged by other researchers. The free downloads at the bottom of this post include three honest slide decks that walk through the debate and offer a synthesis. The short version is this: the clinical model (safety, co-regulation, de-shaming survival responses, state awareness) is robust and useful, even where the specific neuroscience remains contested. A lens, not a law.
With that said, here is what actually works in session.
STATE BEFORE STRATEGY
The most common mistake in nervous system work is not using the wrong tool. It is reaching for any tool before knowing what state you are working with.
The Polyvagal Ladder gives us three working states. At the top sits ventral vagal: calm, connected, curious, open to learning and relationship. This is where therapy does its best work. In the middle is sympathetic activation: mobilised, anxious, restless, scanning for threat, with thinking that becomes narrow and urgent. At the bottom sits dorsal vagal: collapsed, numb, disconnected, foggy. The body has moved into shutdown as a last-resort protection. Clients here often describe it as "I just went blank" or "I stopped caring about anything."
There are also blended states that matter clinically. Wired but numb (sympathetic plus dorsal) produces the burnt-out, running-on-empty presentation. Freeze (sympathetic plus dorsal together) shows up as a body that is tensed and panicked but cannot move or speak. Fawning or pleasing on the outside while collapsed inside is a ventral mask over dorsal shutdown. These blended states are common in clients with complex or relational trauma, and are often misread as disengagement or non-compliance.
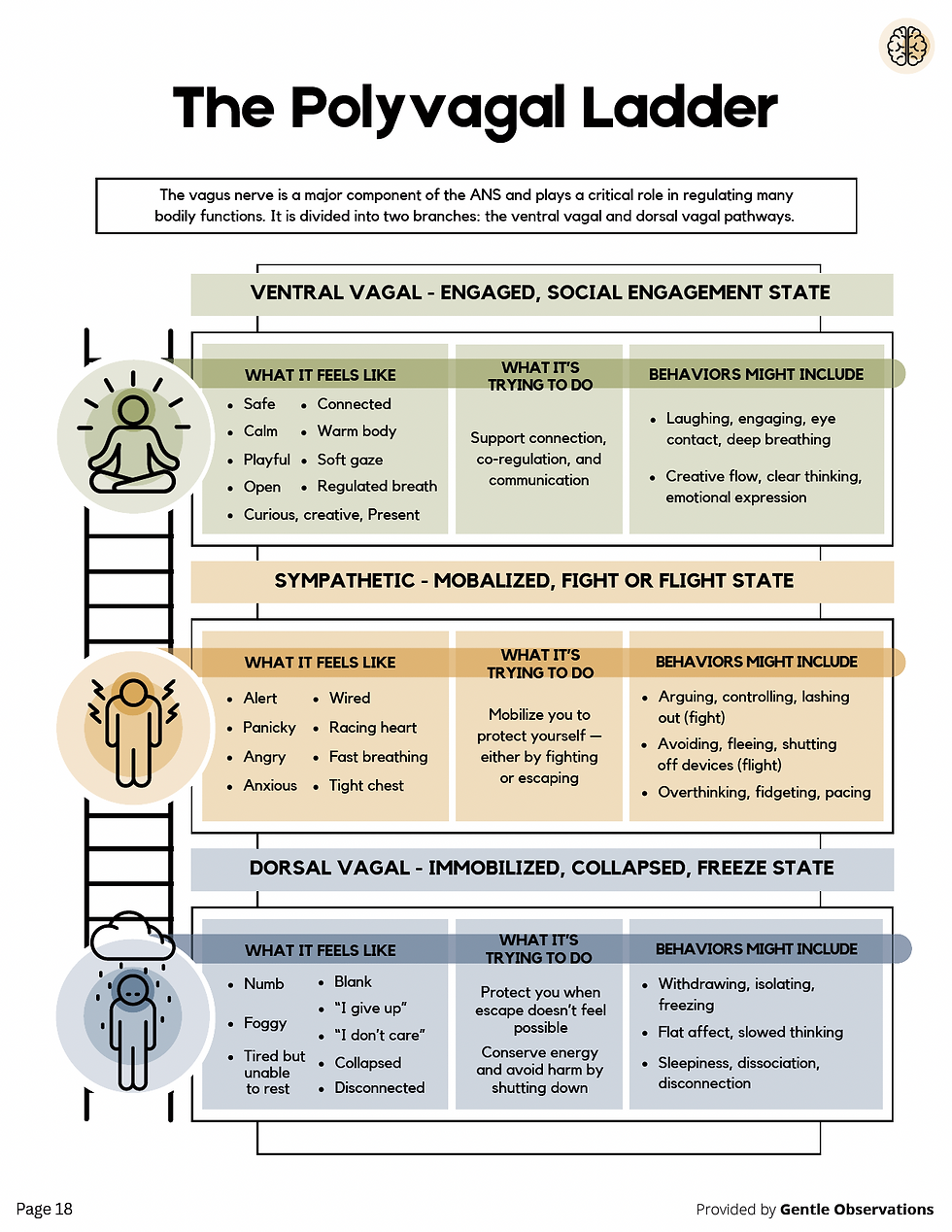
The goal of regulation work is not to keep clients permanently at the top. The Nervous System Toolkit puts this directly:
"The goal is not to stay at the top all the time, but to learn to move up and down the ladder with more awareness, flexibility, and self-compassion."
Flexibility is the clinical target.
READING THE LADDER IN SESSION

Before reaching for any intervention, you need a quick, accurate read of where the client is right now. The Nervous System Toolkit includes a Decision Tree called "What State Am I In Right Now?" that works as both a therapist's internal guide and a psychoeducation tool for clients.
The tree opens with one question: "Right now, what am I noticing most?"
Three branches follow. If the client seems present, breath is natural, they can make eye contact and engage: likely ventral. Stay curious. Can you anchor this moment with a breath, a word, a brief movement?
If they are restless, tense, wanting to escape or fix something, thinking fast or unable to sit still: likely sympathetic. Is there still energy to act? If yes, sympathetic activation is the frame. If that energy is fading, they may be sliding toward dorsal.
If they seem numb, foggy, collapsed, invisible: likely dorsal vagal. The next question matters here: is there also panic or urgency underneath? If yes, this is a blended state, and the approach shifts accordingly.

This matters because the intervention that helps a sympathetic client often worsens things for a dorsal one. Matching the tool to the state is the whole game.
STATE-MATCHED TOOLS: WHAT WORKS WHERE
For sympathetic activation (wired, edgy, tight, urgent):
The system needs to discharge mobilised energy and receive a signal that the threat has passed. Longer exhales activate the parasympathetic branch directly. The extended exhale technique in the Nervous System Toolkit is simple: inhale for 4 counts, exhale for 6 to 8, repeat slowly. Sighing aloud achieves the same physiological effect with less effort. Other tools that work here: humming on the exhale, a regulation walk (4 steps inhale, 6 steps exhale), cold water splashed on the face or back of the neck, and gentle pressure (hands pressing into thighs or a weighted blanket).
For dorsal shutdown (flat, foggy, low energy, disconnected):
Stillness deepens the dorsal state. The system needs gentle activation, not calming. Sway side to side. Clap a 2-beat pattern and have the client mirror it. Warm drink and slow, warm presence. Sunlight or a window. The Somatic Therapy Coping Skill Cards include the "VOOO" sound toning practice here: a low, sustained "vooo" sound on a long exhale that combines vocal vibration with breath without requiring effort from the thinking brain. The "Drop and Shake" card, a full-body shaking practice, is another activator that moves energy without requiring cognitive engagement.
For blended states (wired and numb):
Begin with co-sighs: three natural sighs together, letting the shoulders drop. This organises the chaos slightly before attempting anything else. Then shift to parallel seating (side by side, no direct eye contact required), a brief warm-tone reading, or co-humming. The Nervous System Toolkit's state-matching cheatsheet notes that the goal for blended states is first to bring the two conflicting signals into some kind of sequence, not to address both at once.
THE VAGUS NERVE TOOLKIT IN PRACTICE
The vagus nerve runs from the brainstem all the way through the throat, lungs, heart, and gut. The workbook describes it as "your body's emotional wiring system," carrying information about what is happening in the body up to the brain, and messages from the brain back down to organs and muscles.
Vagal tone is the fitness level of this system: how efficiently it shifts states and recovers from stress. High vagal tone means the nervous system bounces back quickly from activation. Low vagal tone means the client gets stuck and finds it hard to downshift. The useful clinical point is that vagal tone is trainable, gradually and in ways that do not require full ventral access to begin.
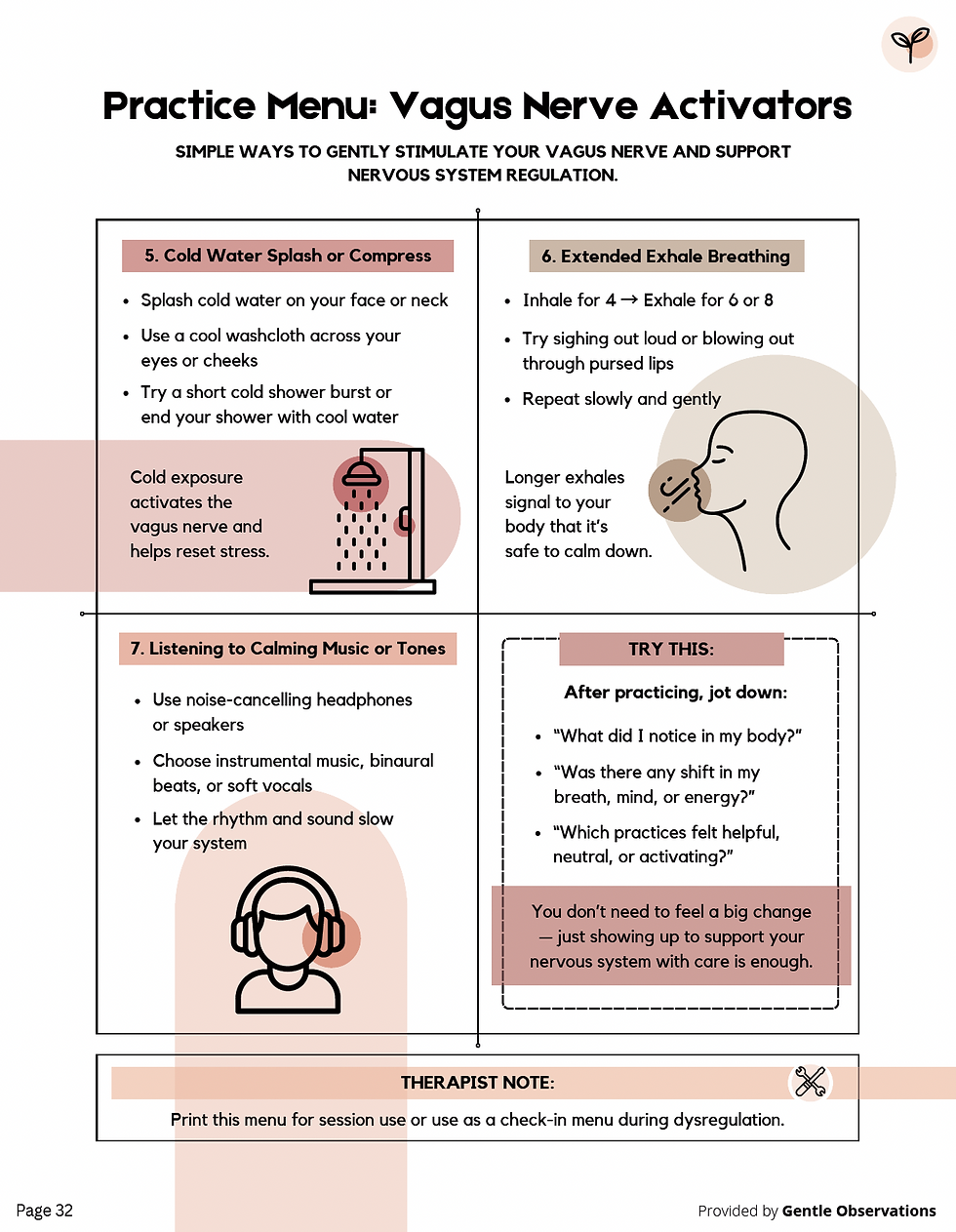
The Practice Menu in the Nervous System Toolkit offers seven practical activator categories. The most versatile for clinical use:
Humming and chanting: slow, low hums on the exhale stimulate the vagal branch near the throat. Even a sustained "mmmm" for 30 seconds gives the body a parasympathetic cue. Easy to introduce in session as a 60-second micro-practice between harder content.
Extended exhale breathing: inhale 4, exhale 6 to 8. The workbook notes: "Longer exhales signal to your body that it's safe to calm down." This is among the most transferable tools for between-session use because it requires no equipment and can be done invisibly.
Gargling: takes 10 to 20 seconds with a sip of water and activates the vagal branch near the larynx and soft palate. Specific enough to be memorable. Practical enough to become a client's go-to morning reset.
Cold water exposure: splashing cold water on the face or neck activates the vagus nerve and helps reset stress physiology. The Nervous System Toolkit recommends ending a shower with a brief cool burst as a daily practice. This is worth introducing carefully with clients who have trauma histories involving cold or water, and contrasting clearly with its mechanism (physiological regulation, not sensory discomfort as a coping method).
Singing and vocal sound: singing softly, even alone, engages the prosody networks that signal safety to the ventral vagal system. Singing in a group is particularly potent for co-regulation. The Somatic Therapy Coping Skill Cards include a "Vocal Toning" card and a "Heal Through Sound" card, both drawing on the same mechanism.

WHEN TRAUMA LOCKS THE LADDER
For clients carrying complex or developmental trauma, the ladder does not move freely. The Nervous System Toolkit calls this "state stickiness": staying in sympathetic or dorsal states longer than the situation warrants. Neuroception, the body's unconscious safety scanner, has been recalibrated by repeated danger. Neutral cues (a flat tone of voice, a notification sound, a closed door) register as threat because the body learned, reasonably, to read the world that way.
The workbook extends the standard fight/flight/freeze model to six trauma responses. This expanded framework is especially useful with clients who cannot identify with "fight or flight" but recognise other patterns immediately:
Fight: body cue is heat in the jaw, loud voice, tight chest. Thought: "I must control this." Micro-exit: exhale longer (4 in, 8 out, five times), press palms into thighs.
Flight: body cue is restless legs, pacing, stomach flutters. Thought: "I have to get out." Micro-exit: regulation walk (4 steps inhale, 6 steps exhale, one to two minutes).
Freeze: body cue is still body with high tension, shallow breath, fixed gaze. Thought: "I can't." Micro-exit: three co-sighs followed by tiny movement, finger taps, ankle circles.
Fawn: body cue is soft voice, smile mask, throat tight. Thought: "Keep the peace." Micro-exit: hand to chest, whisper "My needs matter too."
Flag (submit/yield): body cue is slumped posture, slow speech, heavy limbs. Thought: "Fine. Whatever." Micro-exit: sit 1 cm taller, inhale 4, exhale 6, name one small preference.
Faint (collapse): body cue is dim vision, nausea, cold skin, very low tone. Thought: "I'm gone." Micro-exit: lie or sit with head lowered, slow nasal exhales, warmth or weight anchor, seek medical help if needed.
The reframe the workbook offers for all six: "Your body isn't broken. It learned efficient survival strategies." That single line is worth having on hand as clinical language. It shifts the frame without minimising impact.
THE SOMATIC FLOW: A SESSION-READY SEQUENCE
Section 8 of the Nervous System Toolkit introduces somatic therapy essentials, the foundational mechanics that sit underneath all the specific tools.
Somatic work begins with the body rather than with narrative. The workbook's premise:
"Rather than starting with thoughts and stories, we begin with sensations, breath, posture, movement, and felt safety. The aim isn't to relive the past; it's to update the nervous system in the present, so the body learns new options besides fight/flight/freeze/fawn."
Titration means touching activation in small, manageable amounts. Pendulation means gently moving attention between an activated sensation and a resource or safety cue. Together they teach the nervous system that it can move between states rather than get stuck in one.
The practical sequence the workbook calls the Somatic Flow:
Notice: a cue appears. A breath change, a muscle tightening, a sudden impulse to look away.
Name: the felt sense in two words. Not an emotion label. Something closer to "thick... buzzy... a small knot... heavy cloud." The imprecision is intentional. Naming invites curiosity rather than judgment.
Dose: stay with the sensation for a few breaths without forcing anything. Then pendulate to a resource, a hand on the chest, a steady surface, something warm.
Complete: allow a small impulse to move through. A sigh. A slight stretch. An orienting glance around the room.
End well: use a resource and a closing phrase. "Enough for now."
The workbook closes its instructions with this: "You don't have to 'do it right.' You only need to notice, choose one tiny step, and end well. This is a practice: repeatable over perfect."
That is the frame the whole toolkit operates from. Not mastery. Not eliminating distress. More choice, more safety, more connection, built one small rep at a time.
DOWNLOAD: FREE POLYVAGAL THEORY TOOLKIT
Polyvagal Theory Cheatsheet
Everything you need to introduce the ladder framework, neuroception, and co-regulation to clients or your own practice. One-page format, designed to be handed directly to clients or used as a session reference.
Bonus: Polyvagal Theory Critique Slide Decks (also free)
The science behind polyvagal theory is more contested than most clinical training lets on. These three slide decks walk through the debate, Porges' original claims, Grossman's critique, the questions about dorsal vagal anatomy, and a synthesis that keeps what is clinically useful while being honest about what remains uncertain.
If you use PVT regularly with clients, these are worth reading. If you have been skeptical of the framework, they might give you a more nuanced place to land.
Mechanism or Metaphor?

Scientific Fact or Useful Metaphor?
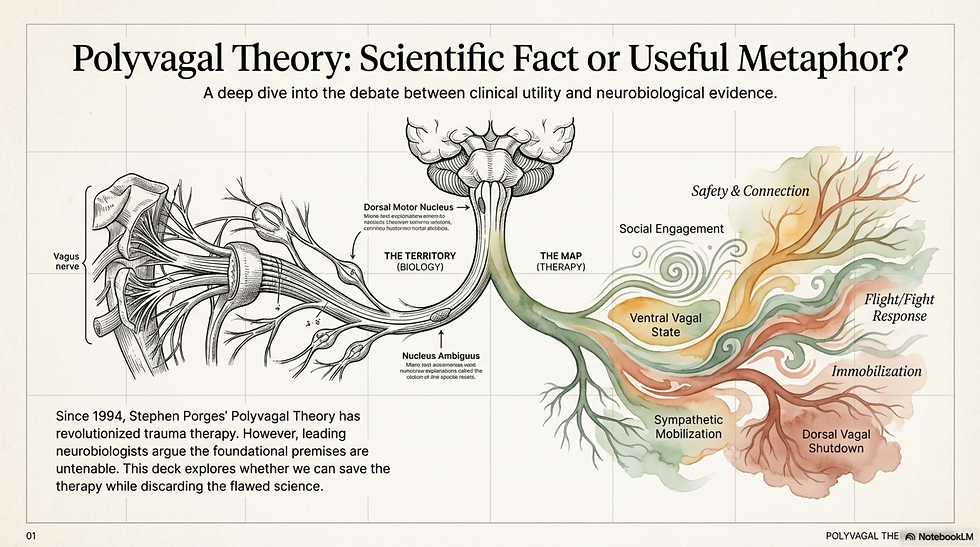
The Polyvagal Paradox

MORE NERVOUS SYSTEM AND SOMATIC TOOLS IN THE LIBRARY
The Nervous System Toolkit: 110 pages across 10 sections, from ANS basics through somatic therapy essentials and polyvagal-informed goal setting. Built for therapists to use in session and assign between sessions.
Somatic Therapy Coping Skill Cards: 30 body-based regulation tools in card format. State-matched, session-ready, designed to be handed directly to clients.
The Nervous System Toolkit and Somatic Therapy Coping Skill Cards are both inside the Library, alongside 1000+ other clinically grounded, session-ready resources. If you want everything in one place, this is where it lives.
Jemma (Gentle Observations Team)

I'm Jemma, a professionally trained mental health professional and digital product creator. I've built a profitable therapy resource business from my clinical expertise. I teach other therapists to do the same, using AI tools that are safe, practical, and built for the way clinicians actually think.






















Comments